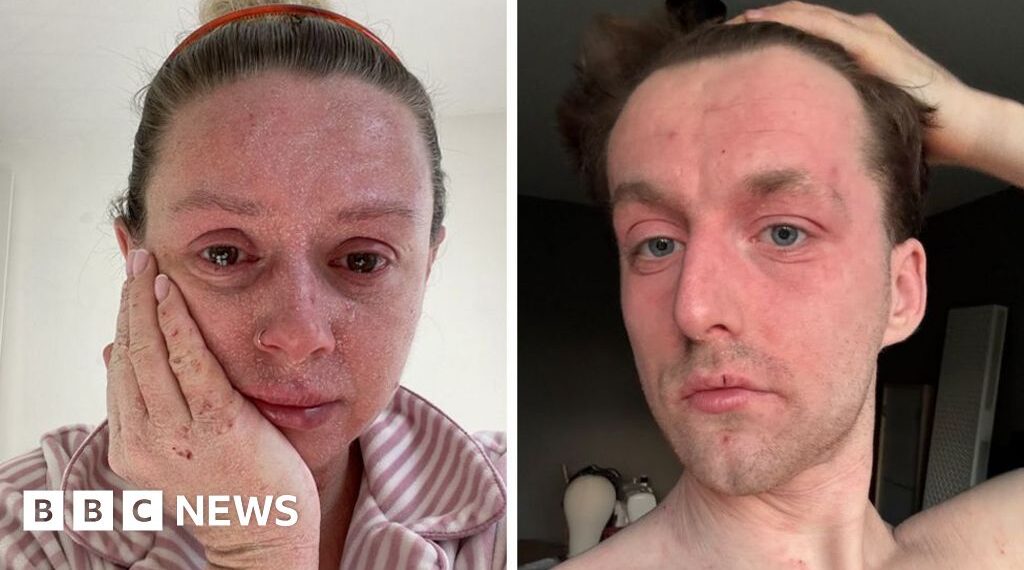
The Critical Challenge of Diagnosing Topical Steroid Withdrawal Across Diverse Skin Phenotypes
Topical Steroid Withdrawal (TSW), a complex and often debilitating condition arising from the cessation of mid-to-high potency topical corticosteroids, has emerged as a significant point of contention and study within the global dermatological community. Characterized by widespread inflammation, skin barrier dysfunction, and intense pruritus, TSW,sometimes referred to as Red Burning Skin Syndrome,presents a multifaceted diagnostic challenge. This challenge is significantly exacerbated by a historical clinical focus on Caucasian skin tones, which often serves as the “standard” for medical education and diagnostic criteria. As the medical community grapples with the rising prevalence of this condition, it is becoming increasingly clear that the inability to recognize TSW in patients of color is not merely a clinical oversight but a systemic failure in healthcare equity and diagnostic accuracy.
The pathophysiological underpinnings of TSW involve the downregulation of corticosteroid receptors and the subsequent vasodilation of cutaneous blood vessels once the suppressive agent is removed. While the physiological mechanism remains consistent across all human biology, the visual manifestation of this inflammatory response is heavily mediated by the concentration and distribution of melanin. Consequently, the reliance on traditional descriptors such as “erythema” (redness) fails to capture the clinical reality for a significant portion of the global population, leading to prolonged suffering and inappropriate medical interventions.
The Spectrum of Inflammation: Beyond the “Red Skin” Paradigm
In the traditional medical literature, TSW is frequently described as “Red Skin Syndrome.” While this terminology is descriptive for patients with lower levels of melanin, it is fundamentally exclusionary for those with darker skin tones. On white or light-olive skin, the hallmarks of TSW include a bright, confluent erythema that often stops abruptly at the wrists or ankles (the “sleeve sign”). However, in patients with Black or Brown skin, the inflammatory response does not manifest as a bright red glow. Instead, the increased blood flow and tissue distress present as deep shades of purple, dark brown, or even a distinctive grayish, ashen tinge.
This chromatic variance is due to the way melanin absorbs and scatters light. When significant inflammation occurs in melanated skin, the underlying redness is masked by the pigment, resulting in hyperpigmentation or a “dusky” appearance. When clinicians are trained primarily using imagery of “bright red” inflammation, they frequently misinterpret these deeper hues as post-inflammatory hyperpigmentation or simply as a worsening of the original eczema. This misinterpretation is a critical junction in the patient’s journey; failing to recognize the “deep purple” or “grayish” indicators of TSW often leads to the prescription of even stronger corticosteroids, effectively trapping the patient in a cycle of dependency and escalating physiological damage.
Clinical Impediments and the Risks of Pharmacological Over-Prescription
The diagnostic discrepancy between skin tones creates a dangerous feedback loop in pharmacological management. When a patient of color presents with the “grayish” or “purple” inflammation characteristic of TSW, and the clinician fails to identify it as such, the standard response is often to escalate treatment. This usually involves prescribing higher-potency topical steroids or systemic immunosuppressants, under the assumption that the patient is suffering from “recalcitrant” or “steroid-resistant” atopic dermatitis.
This mismanagement carries heavy economic and physiological costs. For the patient, the continued application of corticosteroids further thins the dermis and deepens the vascular addiction. For the healthcare system, this represents an inefficient use of resources, leading to increased specialist consultations, emergency room visits for secondary infections, and a loss of productivity for the patient. Furthermore, the psychological toll on patients who feel their symptoms are being ignored or misunderstood cannot be overstated. The “invisible” nature of their inflammation in the eyes of a classically trained clinician often leads to a breakdown in the patient-provider relationship, driving many individuals toward unsupervised “cold turkey” withdrawal methods that can lead to severe systemic complications.
Structural Reforms in Medical Education and Visual Literacy
Addressing the diagnostic gap in TSW requires a fundamental shift in medical education and visual literacy. For decades, dermatological textbooks have been overwhelmingly populated with images of white skin. This has created a “visual bias” where medical students and residents are conditioned to look for a specific chromatic response to diagnose inflammation. To provide equitable care, the industry must prioritize the inclusion of diverse skin phenotypes in all levels of medical training. Clinical guidelines for TSW must be updated to explicitly describe the manifestations of withdrawal in melanated skin, replacing the singular focus on “redness” with a broader spectrum of inflammatory markers.
Moreover, the integration of advanced diagnostic technologies could mitigate human error in visual assessment. Tools such as cross-polarized photography and multispectral imaging can help clinicians see beyond the melanin layer to assess the underlying vascular status. However, technology is only a partial solution. The primary objective must be a cultural and educational shift toward “inclusive dermatology.” By normalizing the appearance of purple, brown, and gray inflammation in the clinical setting, the medical community can ensure that TSW is caught early, reducing the duration of patient suffering and preventing the long-term cutaneous damage associated with prolonged steroid misuse.
Concluding Analysis: The Imperative for Diagnostic Precision
Topical Steroid Withdrawal is a condition that challenges our current understanding of dermatological therapy and patient safety. The nuance of its presentation across different skin tones serves as a poignant reminder that medical “standards” are often built upon a narrow demographic foundation. The authoritative consensus must now move toward a more sophisticated, inclusive diagnostic framework. Recognizing that TSW manifests as purple or gray in Black and Brown patients is not merely a matter of clinical curiosity; it is a prerequisite for competent medical practice.
As we look toward the future of dermatological care, the focus must remain on precision and equity. Regulatory bodies and professional organizations must lead the charge in redefining diagnostic criteria to be inclusive of all skin tones. Failure to do so will result in a continued “diagnostic shadow” for patients of color, where severe inflammatory conditions are overlooked due to a lack of visual representation in the clinical canon. Ultimately, the goal is to foster a healthcare environment where the color of a patient’s skin does not dictate the accuracy of their diagnosis or the efficacy of their treatment path.